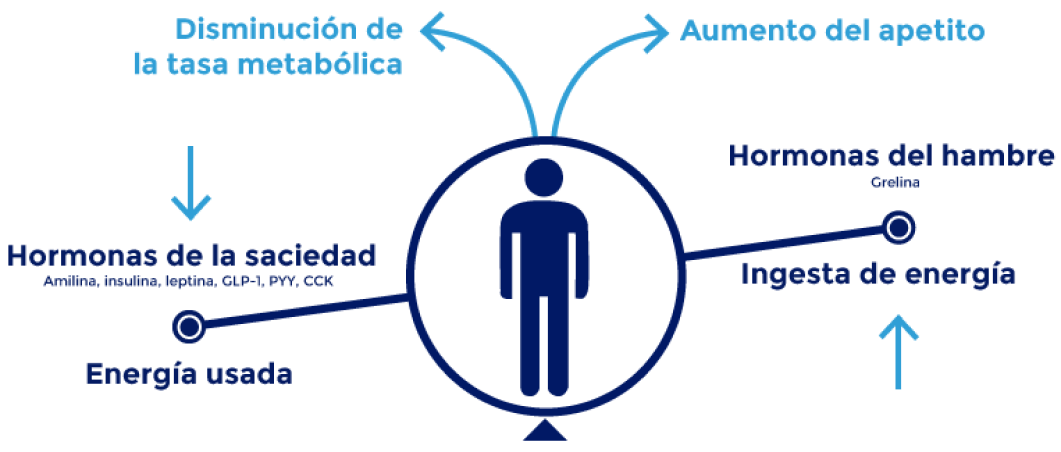
La obesidad se debe tratar de forma integral y como una enfermedad crónica grave10 47.
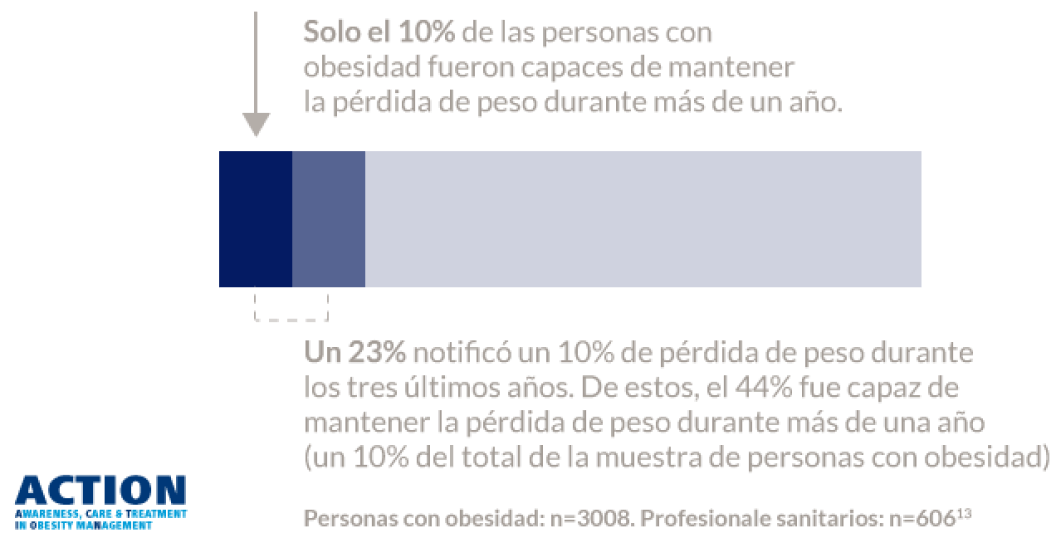
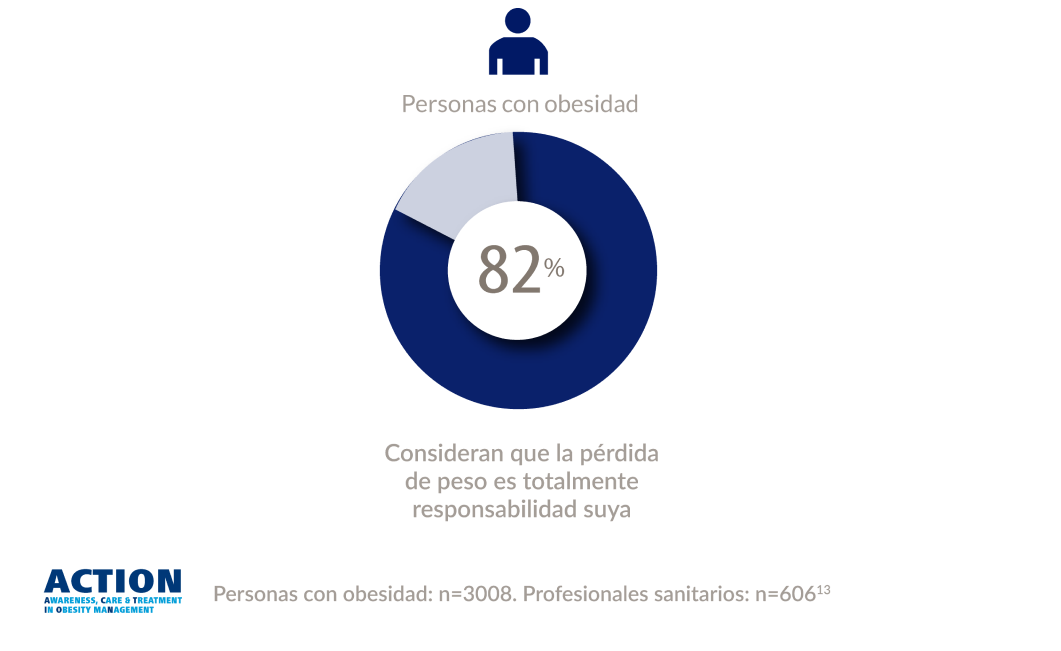
Solo un 55 % de las personas con obesidad informan haber sido diagnosticadas de obesidad. Entre los que hablaron sobre el peso con su profesional sanitario, solo el 24 % informó de que se había programado una cita de seguimiento relacionada con el peso13.
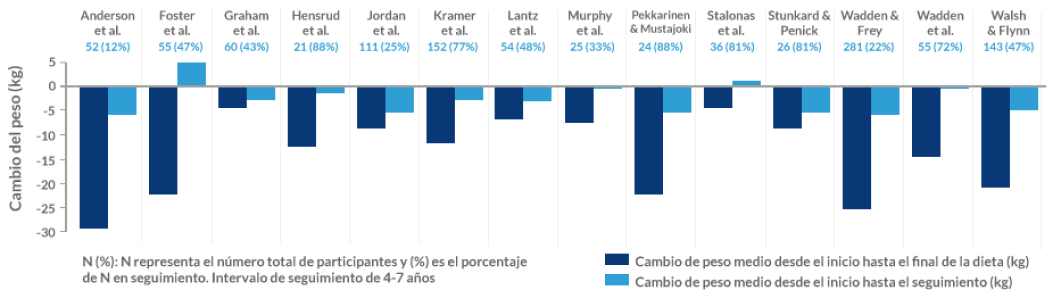
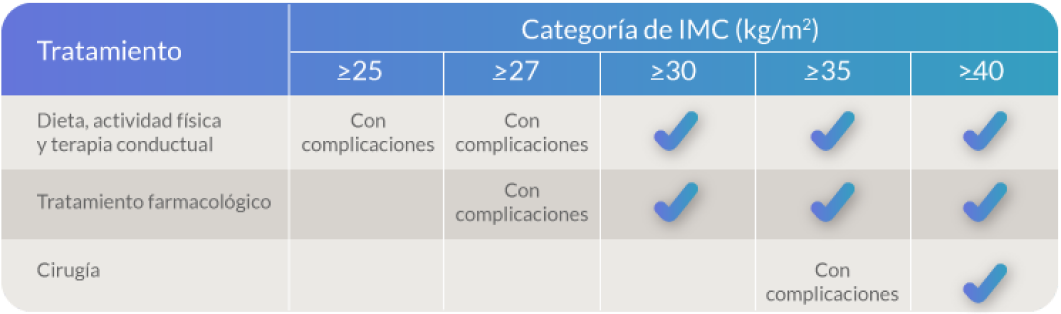
Tratamiento de estilo de vida basado en datos científicos: el tratamiento para la obesidad debe incluir dieta, ejercicio y modificación de la conducta47. Alimentación sana, actividad física y terapia conductual deben ser intervenciones de primera línea en todas las personas con un IMC ≥ 25 kg/m2 y deben formar parte de cualquier intervención para la pérdida de peso . Sin embargo, estas intervenciones no siempre son suficientes para mantener la pérdida de peso45,48.
Tratamiento farmacológico: el tratamiento con fármacos para la obesidad se puede considerar si el tratamiento de estilo de vida no proporciona suficientes beneficios clínicos a las personas con un IMC 30 kg/m2, o 27 kg/m2 con complicaciones relacionadas con la obesidad.48 Algunos de los medicamentos aprobados para el control de peso pueden actuar directamente sobre el sistema nervioso central, induciendo la pérdida de peso mediante la reducción de apetito, o actuar de manera periférica e inducir la pérdida de peso por interferir con la absorción por parte del sistema gastrointestinal.49
Procedimientos bariátricos: son la intervención de tercera línea para el tratamiento de la obesidad, que se recomienda en personas con un IMC 40 kg/m2 , o 35 kg/m2 con comorbilidades. La cirugía bariátrica puede ser malabsortiva (produce mala absorción de los alimentos) o restrictiva, y cada tipo requiere de diferentes cambios en el estilo de vida.50
1. Wright SM, Aronne LJ. Causes of obesity. Abdominal Imaging. 2012; 37:730–732.
2. National Institutes of Health. Clinical Guidelines On The Identification, Evaluation, And Treatment Of Overweight And Obesity In Adults. Disponible en: http://www.nhlbi.nih.gov/guidelines/obesity/ob_gdlns.pdf. Último acceso: marzo de 2018.
3. NIH. What causes overweight and obesity? Disponible en: https://www.nhlbi.nih.gov/health/healthtopics/topics/obe/causes. Último acceso: marzo de 2018.
4. Sumithran P PL, Delbridge E, Purcell K, Shulkes A, Kriketos A, Proietto J. Long-term persistence of hormonal adaptations to weight loss. New England Journal of Medicine. 2011; 365:1597–1604.
5. Collins J, JE B. Behavioral and Psychological Factors in Obesity. The Journal of Lancaster General Hospital. 2009; 4:124–127
6. Pampel FC, Denney JT, PM K. Obesity, SES, and economic development: a test of the reversal hypothesis. Social science and medicine. 2013; 74:1073-1081.
7. WHO. Obesity: Preventing and managing the global epidemic. Disponible en: http://www.who.int/iris/handle/10665/42330 Último acceso: marzo de 2018.
8. Allison DB, Downey M, Atkinson RL, et al. Obesity as a Disease: A White Paper on Evidence and Arguments Commissioned by the Council of The Obesity Society. Obesity. 2008; 16:1161–1177.
9. American Medical Association. A.M.A Adopts New Policies on Second Day of Voting at Annual Meeting. Obesity as a Disease. Disponible en: http://news.cision.com/american-medical-association/r/ama-adopts-new-policies-onsecond-day-of-voting-at-annual-meeting,c9430649. Último acceso: marzo de 2018.
10. Mechanick JI, Garber AJ, Garvey WT. American Association of Clinical Enodocrinologists’ Position Statement on Obesity and Obesity Medicine. Endocrine Practice. 2012; 18:642-648.
11. Bray G, Kim K, Wilding J. Obesity: a chronic relapsing progressive disease process. A position statement of the World Obesity Federation. Obesity Reviews. 2017; 18:715–723.
12. Frühbeck G, Sbraccia P, Nisoli E. 2015 Milan Declaration: A Call to Action on Obesity – an EASO Position Statement on the Occasion of the 2015 EXPO. Obesity Facts. 2016; 9:296-298.
13. Kaplan L, Golden A, Jinnett K, et al. Perceptions of Barriers to Effective Obesity Care: Results from the National ACTION Study. Obesity. 2018; 26:61-69
14. Lobstein T, Brinsden H, Gill T, et al. Comment: obesity as a disease – some implications for the World Obesity Federation’s advocacy and public health activities. Obesity reviews. 2017; 18:724–726
15. World Health Organization. Obesity and Overweight Factsheet no. 311. Disponible en: http://www.who.int/mediacentre/factsheets/fs311/en/. Último acceso: marzo de 2018.
16. Global Health Observatory. Prevalence of Obesity, ages 18+, 2016 (age standardized estimate) Male. Disponible en: http://gamapserver.who.int/mapLibrary/Files/Maps/Global_Obesity_2016_Male.png. Último acceso: marzo de 2018.
17. Global Health Observatory. Prevalence of Obesity, ages 18+, 2016 (age standardized estimate) Female. Disponible en: http://gamapserver.who.int/mapLibrary/Files/Maps/Global_Obesity_2016_Female.png. Último acceso: marzo de 2018.
18. De Lorenzo, A., Gratteri, S., Gualtieri, P., Cammarano, A., Bertucci, P., & Di Renzo, L. (2019). Why primary obesity is a disease?. Journal of translational medicine, 17(1), 1-13.
19. Romero-Corral A, Caples SM, Lopez-Jimenez F, et al. Interactions between obesity and obstructive sleep apnea:implications for treatment. Chest. 2010; 137:711-719.
20. Saydah S, Bullard KM, Chen Y, et al. Trends in Cardiovascular Disease Risk Factors by Obesity Level in Adults in the United States, NHANES 1999-2010. Obesity. 2014; 22:1888–1895.
21. Health Effects of Overweight and Obesity in 195 Countries over 25 Years. New England Journal of Medicine. 2017.
22. Guh DP, Zhang W, Bansback N, et al. The incidence of co-morbidities related to obesity and overweight: a systematic review and meta-analysis. BMC Public Health. 2009; 9:1-20.
23. Centers for Disease Control and Prevention. Cancers Associated with Overweight and Obesity Make up 40 percent of Cancers
24. World Obesity Federation. Healthcare cost of consequences of high BMI. Disponible en: http://docs.wixstatic.com/ugd/6599c5_2a8fa0968efd4854b74f399abb3078c0.pdf?index=true. Último acceso: marzo de 2018.
25. World Heart Federation. The costs of CVD. Disponible en: http://www.championadvocates.org/en/championadvocates-programme/the-costs-of-cvd. Último acceso: marzo de 2018.
26. Knowler WC, Barrett-Connor E, Fowler SE, et al. Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. The New England Journal of Medicine. 2002; 346:393–40
27. Wing RR, Lang W, Wadden TA, et al. Benefits of modest weight loss in improving cardiovascular risk factors in overweight and obese individuals with type 2 diabetes. Diabetes Care. 2011; 34:1481–1486.
28. Dattilo AM, Kris-Etherton PM. Effects of weight reduction on blood lipids and lipoproteins: a meta-analysis. The American Journal of Clinical Nutrition. 1992; 56:320–328.
29. Riddle DL, PW S. Body Weight Changes and Corresponding Changes in Pain and Function in Persons With Symptomatic Knee Osteoarthritis: A Cohort Study. Arthritis Care & Research. 2013; 65:15–22.
30. Tuomilehto H, Seppa J, Uusitupa M, et al. The impact of weight reduction in the prevention of the progression of obstructive sleep apnea: an explanatory analysis of a 5-year observational follow-up trial. Sleep Medicine. 2014; 15:329–335.
31. Foster GD, Borradaile KE, Sanders MH, et al. A randomized study on the effect of weight loss on obstructive sleep apnea among obese patients with type 2 diabetes: the Sleep AHEAD study. Archives of Internal Medicine. 2009; 169:1619–1626.
32. Warkentin LM, Das D, Majumdar SR, et al. The effect of weight loss on health-related quality of life: systematic review and meta-analysis of randomized trials. Obes Rev. 2014; 15:169-182.
33. Kuna ST, Reboussin DM, Borradaile KE, et al. Long-term effect of weight loss on obstructive sleep apnea severity in obese patients with type 2 diabetes. Sleep. 2013; 36:641–649A.
34. Wright F, Boyle S, Baxter K, et al. Understanding the relationship between weight loss, emotional well-being and health-related quality of life in patients attending a specialist obesity weight management service. J Health Psychol. 2013; 18:574-586.
35. Whitlock G, Lewington S, Sherliker P, et al. Body-mass index and cause-specific mortality in 900 000 adults: collaborative analyses of 57 prospective studies. Lancet. 2009; 373:1083-1096.
36. National Obesity Observatory. Obesity and Mental Health. 2011. Disponible en: https://khub.net/c/document_library/get_file?uuid=18cd2173-408a-4322-b577-6aba3354b7ca&groupId=31798783. Último acceso: marzo de 2018.
37. Hopman WM BCJL, Barr SI, Gao Y, Prior JC, Poliquin S, Towheed T, Anastassiades T. The association between body mass index and health-related quality of life: data from CaMos, a stratified population study. Qual Life Res. 2007; 16:1595-1603.
38. Syddall H, Martin H, Harwood R, et al. The SF-36: a simple, effective measure of mobility-disability for epidemiological studies. J Nutr Health Aging. 2009; 13:57–62.
39. Schwartz A, Doucet E. Relative changes in resting energy expenditure during weight loss: a systematic review. Obesity Review. 2010; 11:531–547.
40. Sumithran P, J P. The defence of body weight: a physiological basis for weight regain after weight loss. Clin Sci (Lond). 2013; 124:231–241
41. Rosenbaum M, RL L. Adaptive thermogenesis in humans. Int J Obes (Lond). 2010; 34 (suppl 1):S47–S55.
42. Rosenbaum M, Kissileff HR, Mayer LE, et al. Energy intake in weight-reduced humans. Brain Res. 2010; 1350:95-102.
43. Greenway F. Physiological adaptations to weight loss and factors favouring weight regain. International Journal of Obesity. 2015; 39:1188-1196
44. Lenard N, Berthoud H. Central and Peripheral Regulation of Food Intake and Physical Activity: Pathways and Genes. Obesity. 2008; 16(Suppl 3):S11-S12.
45. Mann T, Tomiyama AJ, Westling E, et al. Medicare’s search for effective obesity treatments: diets are not the answer. The American Psychologist. 2007; 62:220–233.
46. MacLean PS, Wing RR, Davidson T, et al. NIH working group report: Innovative research to improve maintenance of weight loss. Obesity (Silver Spring). 2015; 23:7-15.
47. AACE/ACE. Clinical practice guidelines for comprehensive medical care of patients with obesity – executive summary. Disponible en: https://www.aace.com/files/guidelines/ObesityExecutiveSummary.pdf. Último acceso: marzo de 2018.
48. Jensen MD, Ryan DH, Apovian CM, et al. 2013 AHA/ACC/TOS guideline for the management of overweight and obesity in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and The Obesity Society. Circulation. 2014; 129:S102-138.
49. Mingfang L, B C. Pharmacotherapy for obesity. British Journal of Clinical Pharmacology. 2009; 68:804–810.
50. Obesity Action Coalition. Bariatric surgery. Disponible en: http://www.obesityaction.org/obesitytreatments/bariatric-surgery. Último acceso: marzo de 2018.